
Diagnosis of Canine Babesiosis
Babesiosis is a significant global, mainly tick transmitted disease, caused by various species of the intraerythrocytic protozoan parasite of the genus Babesia. The species most common in naturally infect dogs are, B. canis, vogeli and rossi all a large Babesia species, and B. gibsoni which is a small Babesia species.
Infection can range from asymptomatic to severe, developing into a life-threatening illness.
The primary pathogenesis of babesiosis is hemolytic anemia which is caused by direct erythrocyte injury by the parasites and, in some cases by immune-mediated mechanisms.
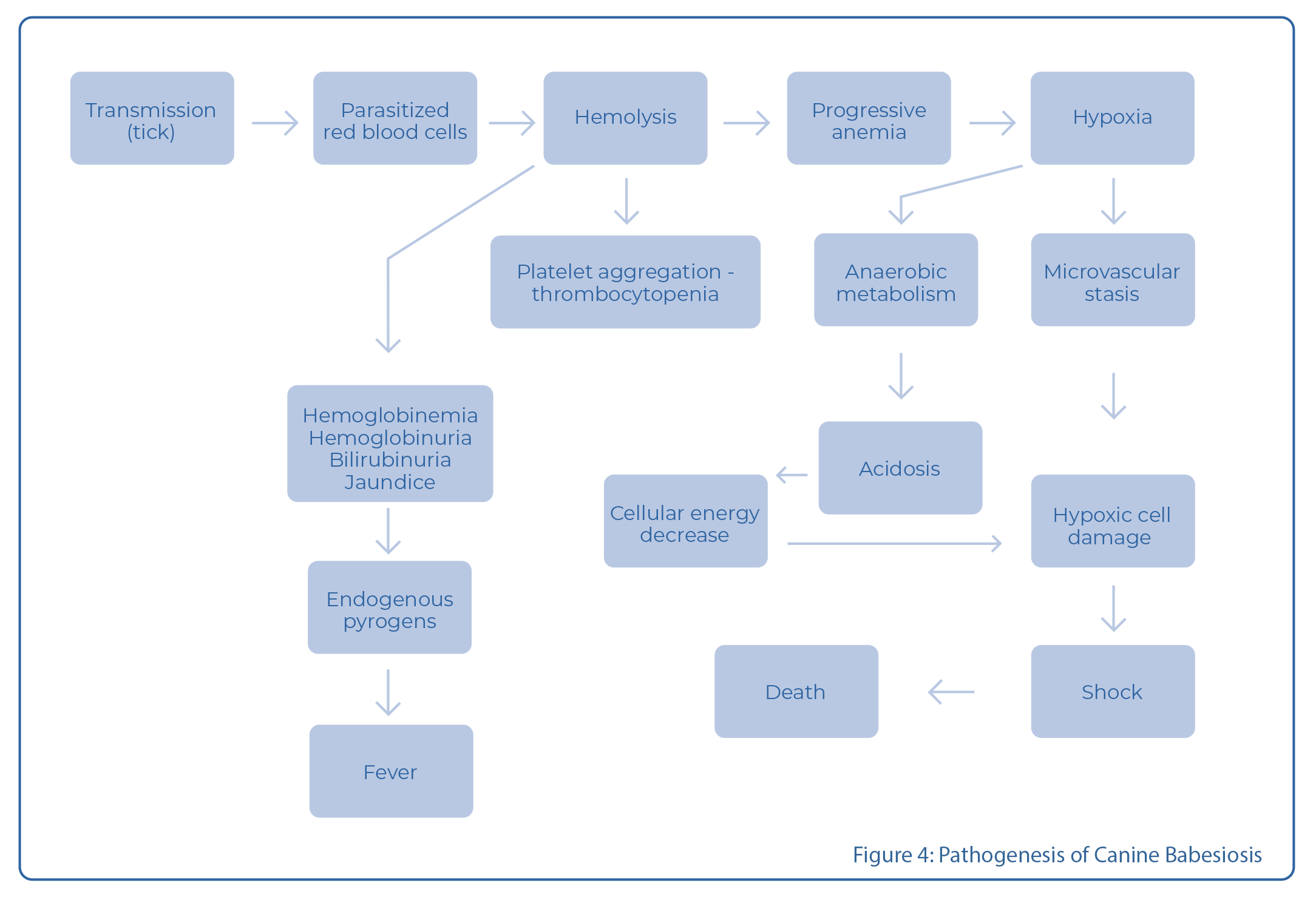
Additional signs include fever, splenomegaly and thromobocytopenia. Babesiosis is a major concern in dogs due to its frequency and severity. The effects can be due to the Babesia infections themselves or coinfections with other agents, in particular Ehrlichia canis, Anaplasma platys and Leishmania infantum.
From a clinical point of view, we may suspect a case of babesiosis in dogs that have a record of tick infections, especially when young, and which are febrile, apathetic, and anorectic, with pale mucous membranes and jaundice. These signs, while suggestive, must be followed by laboratory tests which include species confirmation in order to provide the appropriate treatment for the identified target species.
Babesiosis was traditionally diagnosed by identifying intraerythrocytic trophozoites on stained blood smears, but due to low sensitivity, more sophisticated laboratory diagnostic tests such as immune fluorescent antibody (IFA), ELISA and PCR tests are now used.
In clinic standardized tests:
Haematology:
Anemia with reticulocytosis (regenerative), anisocytosis, polychromasia, neutrophilic leukocytosis, thrombocytopenia, and giant platelets are strong indicators of infection.
In the first days after infection, anemia tends to be mild, normocytic, and normochromic, though it can become macrocytic, hypochromic, and regenerative with the evolution of the disease. Reticulocytosis is proportional to the severity of the anemia.
The leukocyte count varies and may go from leukocytosis to leukopenia. In our experience, however, leukocytosis with neutrophilia is more frequent and may be related to the acute phase of the disease.
Immune-mediated hemolytic anemia (IMHA) can be evaluated with the tube agglutination test and the Coombs test. These tests should precede a blood transfusion that is sometimes necessary.
Biochemistry (blood):
Hyperbilirubinemia, hyperglobulinemia, hypoalbuminemia, hemoglobinemia, elevated liver enzymes (ALT, AST, FA), serum levels of urea and creatinine, hypokalemia, hyponatremia, hypochloremia, hyperlactatemia, and hypoglycemia will be present as the disease establishes itself.
Urinalysis:
Bilirubinuria, hemoglobinuria, and proteinuria are also common as the disease advances.
Parasitology:
Parasitemia is higher in the acute phase, making the parasites more frequently observable in peripheral blood smears. The blood should be collected from peripheral capillaries, mainly from the tip of the ears or tail. This method is considered to have low sensitivity and is not recommended as a sole diagnostic test. However, microscopy visualization of the parasitic forms, associated with anamnesis, physical aspects, and laboratory tests, can help the clinician determine the most likely species. For instance, B. canis, B. vogeli and B. rossi are typically large, piriform-shaped, and usually seen singly or in pairs, while small, isolated, and annular forms are usually associated with B. gibsoni.
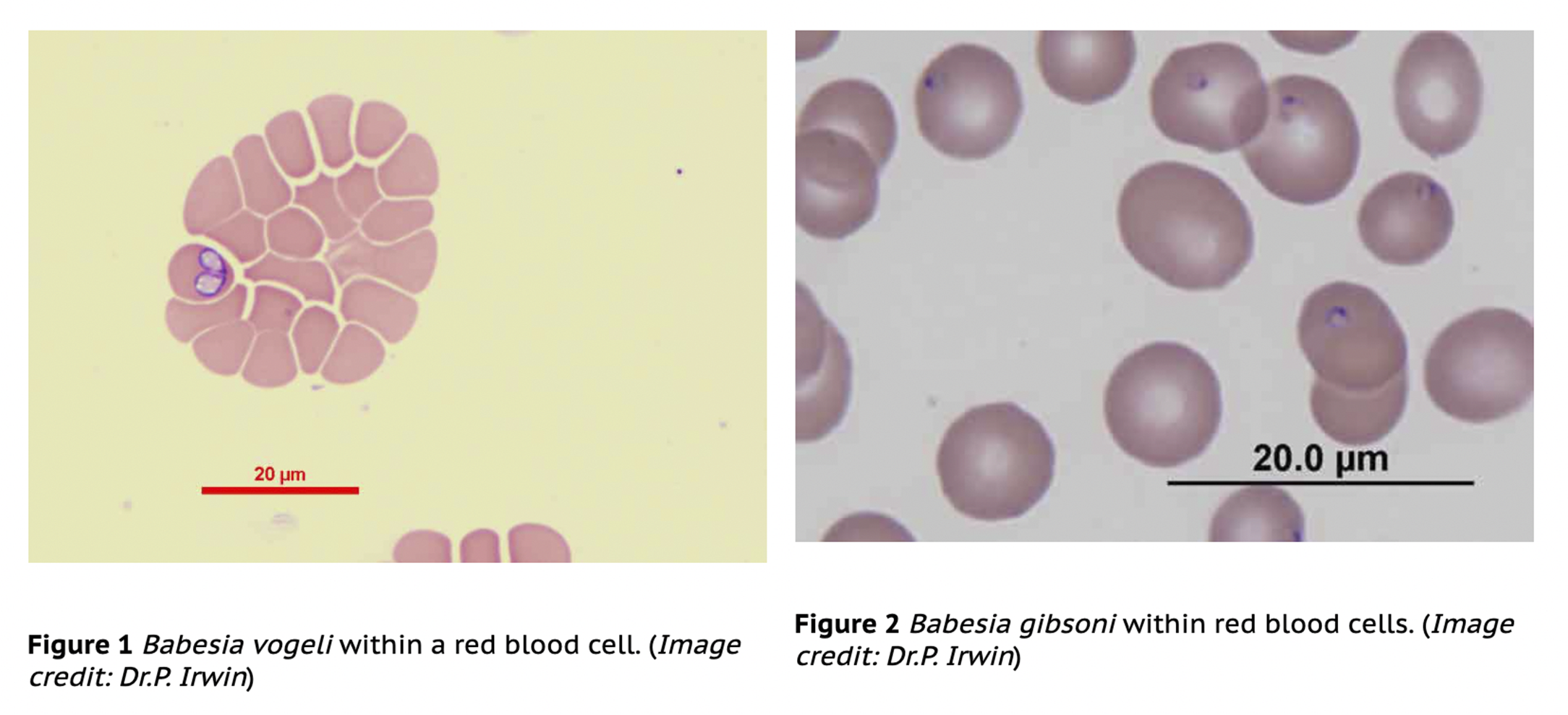
Serological methods: Tests such as immune fluorescent antibody (IFA) and ELISA tests which are employed mostly for epidemiological surveys, require training and specialized equipment. Serological tests are limited in their ability to be used for diagnostic purposes due to:
- False negative results: a positive test result is dependent on the host’s antibody response, which can take up to ten days to develop.
- False Positive: antibody titer levels can remain detectable even after full recovery and therefore can indicate a previous infection. In addition, identification of the organism is complicated by the presence of serological cross reaction between the various species.
Thus, serological testing can be very useful for diagnosing subacute or chronic forms of infection in which the parasites are present in low numbers or absent in the blood. However, many seropositive dogs are clinically normal. In such cases, serology should not be used alone to identify the infection or decide on treatment. Preferably, serologic tests should be applied in paired serum samples taken two or three weeks apart to assess whether antibody titer elevations are consistent with recent infection or active babesiosis.
Molecular Methods:
Molecular techniques allow more reliable species identification, which is important for defining the treatment, besides offering greater sensitivity. PCRs, which are able to accurately detect several vector-transmitted agents, have shown benefits for identifying coinfections, especially ones involving E. canis and A. platys. Another advance linked to molecular examination is in the clinic point-of-care molecular tests such as PCRun (Biogal, Galed Labs). This technique has advantages over standard PCR due to its simplicity and speed (75 minutes – with about 10 minutes hands on). It can be performed in the hospital, clinic, or laboratory environment and has high sensitivity and specificity for identifying different Babesia species.
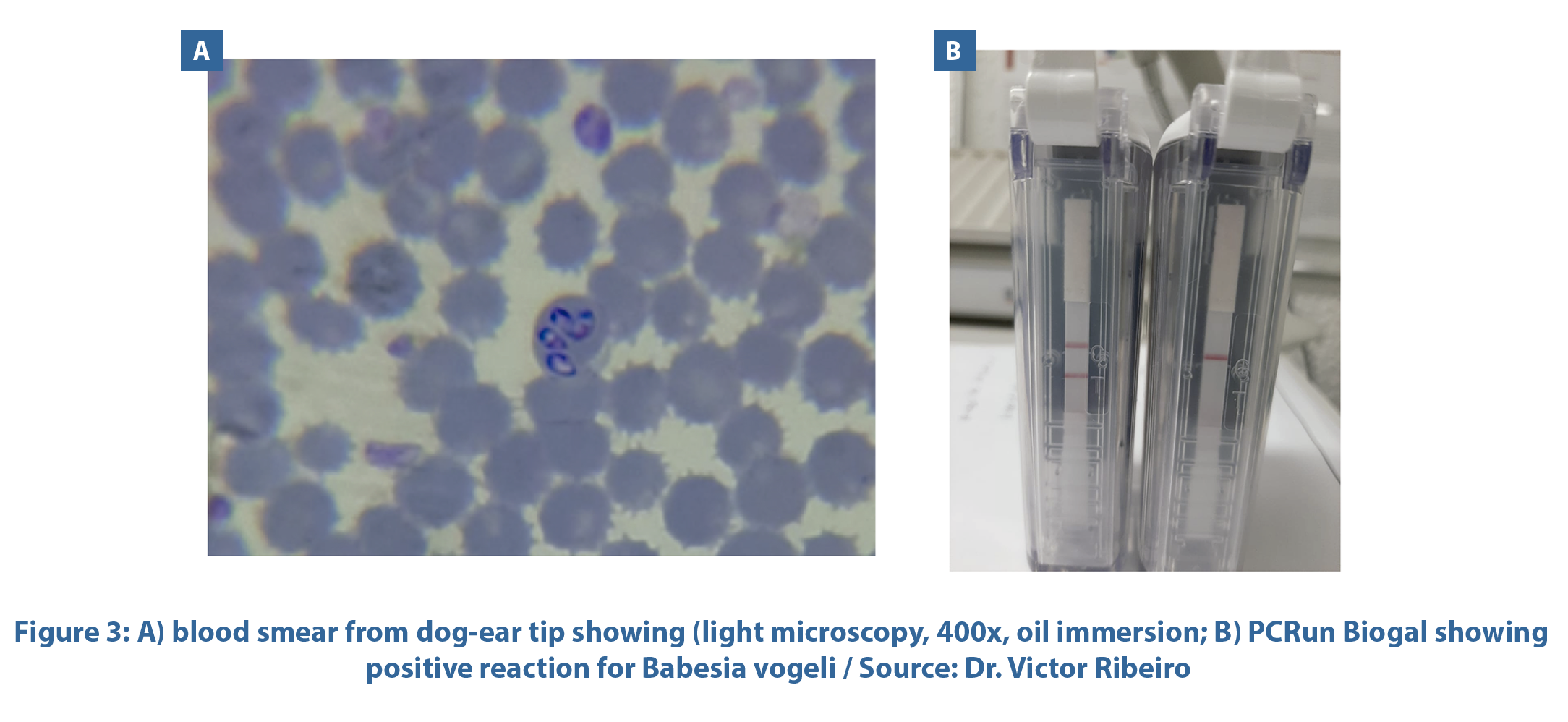
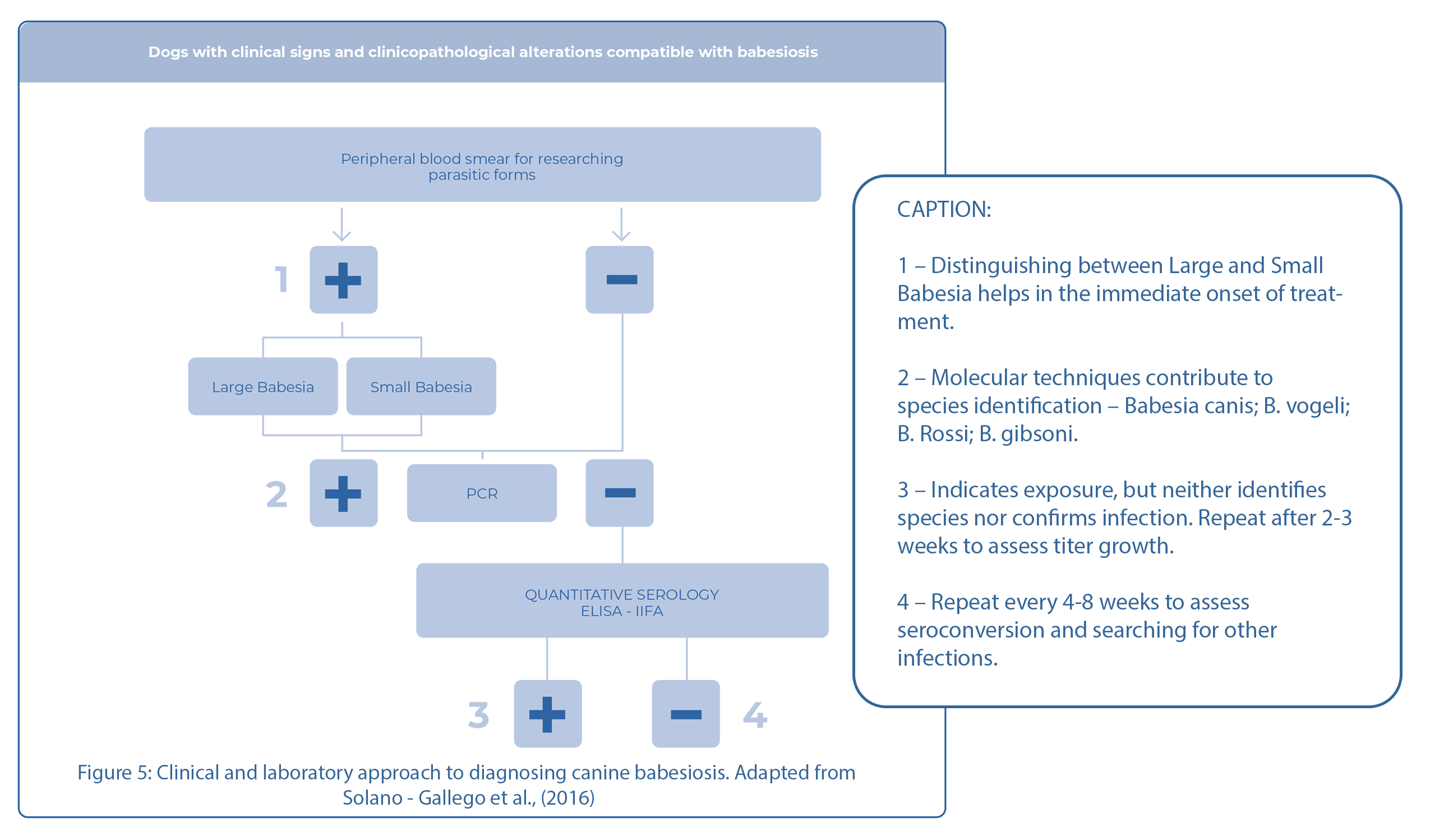
We are aware of gaps in the effective management of canine babesiosis concerning diagnosis, treatment, and control. Veterinarians must be aware of the possible species that can infect dogs and the decision of whether to treat seropositive and even infected animals, depending on the stage of the infection. Another aspect that needs to be understood involves coinfection or positive serology in dogs infected with Leishmania.



